UFit-NPB: Wellness Blog Dispatch

Smooth Movement with Osteoarthritis How Movement, Support, and Small Daily Habits Can Make a Big Difference Osteoarthritis (OA) is more than just "wear and tear" or the occasional stiff joint. It is a chronic condition that changes the environment of your joints, affecting how you move and how you experience your day. For many, OA targets the knees, hips, hands, and spine—making simple activities like climbing stairs, getting out of a car, or even gripping a coffee mug feel more difficult than they used to be. The good news is that while the changes to the joint are permanent, the pain and limitation don't have to be. With a proactive strategy that focuses on protecting your cartilage and strengthening the surrounding muscles, you can regain your confidence and stay active. Many people living with OA find that with the right habits, they can significantly reduce their discomfort and return to the activities they love. What Osteoarthritis Can Feel Like OA symptoms tend to develop gradually over the years. While everyone’s experience is unique, common signs include: Joint aching or deep soreness (especially after activity) Morning stiffness that usually clears up within 30 minutes Stiffness after sitting for long periods (the "movie theater sign") Crepitus (a grinding, popping, or crunching sensation in the joint) Tenderness when applying light pressure to the joint Loss of flexibility or a feeling that the joint is "locked." Bony enlargements (especially in the finger joints) Swelling caused by soft tissue inflammation or extra fluid One of the hallmarks of OA is that it often feels worse at the end of a long day of activity. This is why learning how to "pace" your movement and support your joints is essential. The Role of Exercise and Wellness in Managing OA It’s a common myth that exercise will "wear out" your joints faster. In reality, motion is lotion . Cartilage doesn't have its own blood supply; it relies on joint movement to pump in nutrients and stay healthy. A structured, joint-friendly plan can help: Lubricate the joints to reduce friction and pain Build "Natural Braces" : Strengthening muscles (like the quads for the knee) acts as a shock absorber for the bone. Weight Management : Every pound lost removes four pounds of pressure from your knees. Improve Range of Motion : Keeping the joint moving prevents it from tightening up further. Boost Mood : Managing chronic pain is easier when you feel physically capable and strong. A Simple Movement Prescription for Osteoarthritis The most effective routine for OA isn't about high-intensity training; it’s about consistent, smart movement in these four areas: 1) Low-Impact Cardio (3–5 days/week) Walking, water aerobics, or stationary cycling are perfect. They get the heart pumping and joints moving without the jarring impact of running. Goal: 20–30 minutes at a "conversational" pace. 2) Strategic Strength Training (2–3 days/week) Stronger muscles take the "hit" so your joints don't have to. Focus on: Slow, controlled movements and isometric exercises (holding a position) if full-range movement is currently painful. 3) Daily Range-of-Motion Work Even on your "rest" days, spend 5–10 minutes gently moving your joints through their full available range to prevent morning stiffness from settling in. 4) Balance and Stability (2–3 days/week) OA can sometimes make a joint feel "unstable." Balance exercises improve the communication between your brain and your joints, helping you feel more sure-footed. Living with osteoarthritis shouldn't mean giving up on an active life. If you’re ready to move with less pain and more confidence, coaching can provide the personalized roadmap you need to work with your body, not against it. You don’t have to figure this out alone!

Unlocking Your Knee Joints: Rheumatoid Arthritis Living With Rheumatoid Arthritis: How Movement, Support, and Small Daily Habits Can Make a Big Difference Rheumatoid arthritis (RA) is more than occasional joint pain. It’s a chronic autoimmune condition that can affect how you move, how you feel, and how you live day to day. For many people, RA impacts the hands, wrists, knees, feet, and shoulders—making everyday tasks like opening a jar, getting dressed, walking comfortably, or even sleeping through the night more difficult than they used to be. The good news is that while RA can be challenging, there are proven ways to manage symptoms, protect your joints, and improve your quality of life. With the right approach, many people living with RA feel stronger, more confident, and more in control of their body again. What Rheumatoid Arthritis Can Feel Like RA often shows up differently for each person, but there are several common symptoms that many people experience. The most common symptoms include: Joint pain (especially hands, wrists, knees, and feet) Joint swelling Morning stiffness lasting 30 minutes or longer Warm, tender joints Fatigue and low energy Reduced range of motion and flexibility Weakness (especially grip strength) Symptoms on both sides of the body (symmetrical joint pain) Flare-ups (symptoms come and go, with worse periods) One of the most frustrating parts of RA is its unpredictability. Some days you may feel fine, and other days even simple movement can feel exhausting. That’s why a consistent, joint-friendly strategy is so important. The Role of Exercise and Wellness in Managing RA Many people with rheumatoid arthritis are understandably nervous about exercise. They worry it will make inflammation worse or increase pain. But research and real-life experience show the opposite when movement is done correctly. A safe, structured wellness plan can help: Reduce stiffness Improve mobility Strengthen muscles that support the joints Increase energy over time Improve balance and stability Support heart health (RA can increase cardiovascular risk) Help with weight management, which reduces stress on joints The key is not “pushing harder.” The key is learning how to move in a way that supports your joints. A Simple Movement Prescription for Rheumatoid Arthritis The most effective movement routine for RA typically includes four areas: 1) Low-impact cardio (3–5 days/week) Walking, cycling, swimming, or using the elliptical are excellent choices. A good goal is: 20–40 minutes Moderate intensity: A pace where you can still talk, but you feel like you’re working 2) Strength training (2–3 days/week) Strength training is one of the best ways to protect joints because stronger muscles reduce stress on the joints themselves. Focus on: Full-body strength, Controlled movements, Light to moderate resistance 3) Daily mobility and flexibility Even 5–10 minutes of gentle mobility can reduce stiffness and help joints feel more comfortable. 4) Balance and stability training (2–3 days/week) Balance work improves coordination, stability, and confidence—especially when joints feel unstable. When you live with rheumatoid arthritis, exercise should feel supportive—not punishing. If you’re ready to feel stronger, move with more confidence, and create a wellness plan that works with your joints—not against them—coaching can help. You don’t have to figure this out alone!

When Calcium Crystals Attack: How Hydroxyapatite Deposition Disease (HADD) Steals Your Mobility—and How to Fight Back! Have you ever woken up with searing pain in your shoulder, hip, or knee and wondered how a seemingly healthy joint could suddenly betray you? You might be surprised to learn that tiny calcium crystals—specifically hydroxyapatite—can build up in the tendons and soft tissues around your joint and cause intense, sometimes debilitating pain. This condition is called Hydroxyapatite Deposition Disease (HADD), and it’s more common than many people realize. Why HADD Matters HADD is often mistaken for bursitis, tendonitis, or rotator cuff injuries. Because its onset can be sudden and dramatic, many people rush to imaging centers or emergency rooms for answers. Understanding HADD helps patients get the right diagnosis and faster relief—without unnecessary procedures. What is Hydroxyapatite Deposition Disease? HADD occurs when hydroxyapatite crystals (a form of calcium phosphate) deposit in tendons, bursae, or other soft tissues near joints. The shoulder is the most commonly affected area, particularly the rotator cuff tendons, but HADD can also affect the hip, wrist, elbow, knee, and other sites. Deposits can trigger an acute inflammatory response, producing severe pain, swelling, and restricted movement. Common symptoms Sudden, intense joint pain—often waking people at night. Local swelling and warmth. Severely limited range of motion (e.g., unable to lift your arm). Pain that may come in waves: a painful acute phase followed by weeks of gradual improvement. Symptoms can sometimes mimic an infection, so a medical evaluation is important. Who gets HADD? HADD most often affects adults between 30 and 60 years old, though it can occur at any age. There’s no single known cause, but factors like repetitive microtrauma, metabolic conditions, and local tissue degeneration may contribute. Many patients have no obvious risk factor. How it’s diagnosed? Clinical history and physical exam: doctors note the suddenness and pattern of pain. X-rays: can reveal calcific deposits near the joint. Ultrasound: Excellent for identifying and localizing deposits, as well as guiding injections or procedures. MRI: used if other conditions need to be ruled out. Aspiration/analysis: rarely required; usually, imaging is enough. Treatment options that relieve pain and restore function? The good news is that many people recover well with conservative care. Options include: Rest, ice, and short-term use of NSAIDs for pain control. Corticosteroid injections into the bursa or tendon to reduce inflammation (often ultrasound-guided for accuracy) Physical therapy to restore the range of motion and strengthen the surrounding muscles Ultrasound-guided needle lavage (barbotage): a procedure that breaks up and flushes out the calcium deposit, can provide rapid relief. Extracorporeal shock wave therapy (ESWT): a noninvasive option used in some centers to break up deposits. Arthroscopic surgery: reserved for persistent cases that fail conservative measures. Prognosis and recurrence Many acute HADD episodes are self-limited over weeks to months, especially with targeted therapy. However, deposits can recur or persist; timely treatment improves outcomes and reduces the risk of long-term stiffness. When to seek urgent care? If severe pain is accompanied by fever, spreading redness, or rapidly worsening symptoms, seek immediate medical attention—these signs could indicate infection or another serious condition. Hydroxyapatite Deposition Disease can be frightening when it strikes, but with the right diagnosis and targeted treatment, many people regain full function quickly. If you’ve had sudden, severe joint pain—or repeated “mysterious” flareups—don’t shrug it off. Get informed, check your symptoms, and connect with a provider who knows how to treat HADD effectively.

Navigating the Depths of Depression: A Path Forward Navigating depression is a complex journey that transcends simple sadness, affecting your emotions, physical health, and daily behavior. As of late 2025, modern wellness approaches increasingly emphasize integrated, person-centered care that addresses both the "from the neck up" mental challenges and "from the neck down" physical symptoms. 1. Build Momentum with Small Steps When depression drains your energy, starting with "tiny goals" can prevent overwhelm and build confidence. The 5-Minute Rule: Commit to an activity for just five minutes—such as putting one item away or walking around the block. Often, starting is the hardest part, and movement can generate the motivation you currently lack. Establish Stability: Create a loose but structured routine with consistent sleep and meal times. Simple morning rituals, like getting dressed or drinking water, provide a sense of control. Nature and Grounding: Spending even 15 minutes outside can improve clarity and mood. Use mindfulness techniques to focus on the present moment and help break cycles of negative rumination. 2. The Power of Intentional Wellness Your physical habits can directly influence your brain chemistry. Physical Activity: Regular exercise, particularly rhythmic activities like walking or swimming, releases endorphins and neurotransmitters like serotonin and dopamine. For many, moderate exercise can be as effective as medication for mild to moderate depression. Intentional Eating: Focus on nutrient-dense foods rich in Omega-3 fatty acids and B vitamins. Avoid skipping meals to prevent blood sugar crashes that can exacerbate irritability and fatigue. 3. Connection as a Lifeline Isolation fuels depression, while social support acts as a critical buffer. Seek Social Support: Whether through online communities or trusted friends, sharing your journey helps combat the profound sense of isolation. Perspective Shifts: Shifting from a mindset of "beating" depression to viewing it as a journey of self-discovery can foster long-term resilience. Re-engagement: Restore joy by gradually re-engaging with hobbies or small things that once brought satisfaction. 4. Professional Guidance Recovery is not a linear process and often requires professional help. Collaborative Care: Partnering with physicians and certified health coaches ensures your fitness and lifestyle changes complement medical treatment plans. Evidence-Based Therapy: Professionals can provide structured guidance through Cognitive Behavioral Therapy (CBT) to challenge negative thought patterns or Interpersonal Therapy (IPT) to improve relationship dynamics.

Managing Loneliness as You Age Loneliness is a complex and difficult feeling that can affect anyone at any age. As young adults, we give little thought to getting older and feeling alone. We live each day not considering that the social aspects of our life may not always be as we age. Loneliness can leave you feeling empty, disconnected from the world, fearful of dying with no one around, or even abandoned. Loneliness is often described as a sense of isolation or disconnection from others. It can be caused by a variety of factors such as social isolation, loss of loved ones, or even just a lack of meaningful connections with others. We were never intended to live life alone at any age or life stage. Managing loneliness can be challenging, but several strategies can help you cope with loneliness which include reaching out to loved ones and joining social groups and communities. Engage in activities that bring you joy and fulfillment. Try something new that will require you to step out of your comfort zone. Instead of focusing outwardly on others to fill the void look inward toward yourself. Focus on having a relationship with yourself and usually the law of attraction will occur. Always be kind to those you encounter which can open the door for relationships to develop. Older adults tend to isolate themselves when managing various medical conditions out of fear of judgment, embarrassment, or fear of rejection. Accept and understand that aging and the changes that occur along the way are part of the life cycle. Remember that it's okay to feel lonely, and seeking support from others can make a big difference., such as staying connected with friends and family, engaging in activities that bring joy and fulfillment, and seeking support from mental health professionals when necessary. It's important to remember that feeling lonely is a common experience, and there is no shame in seeking help or support.
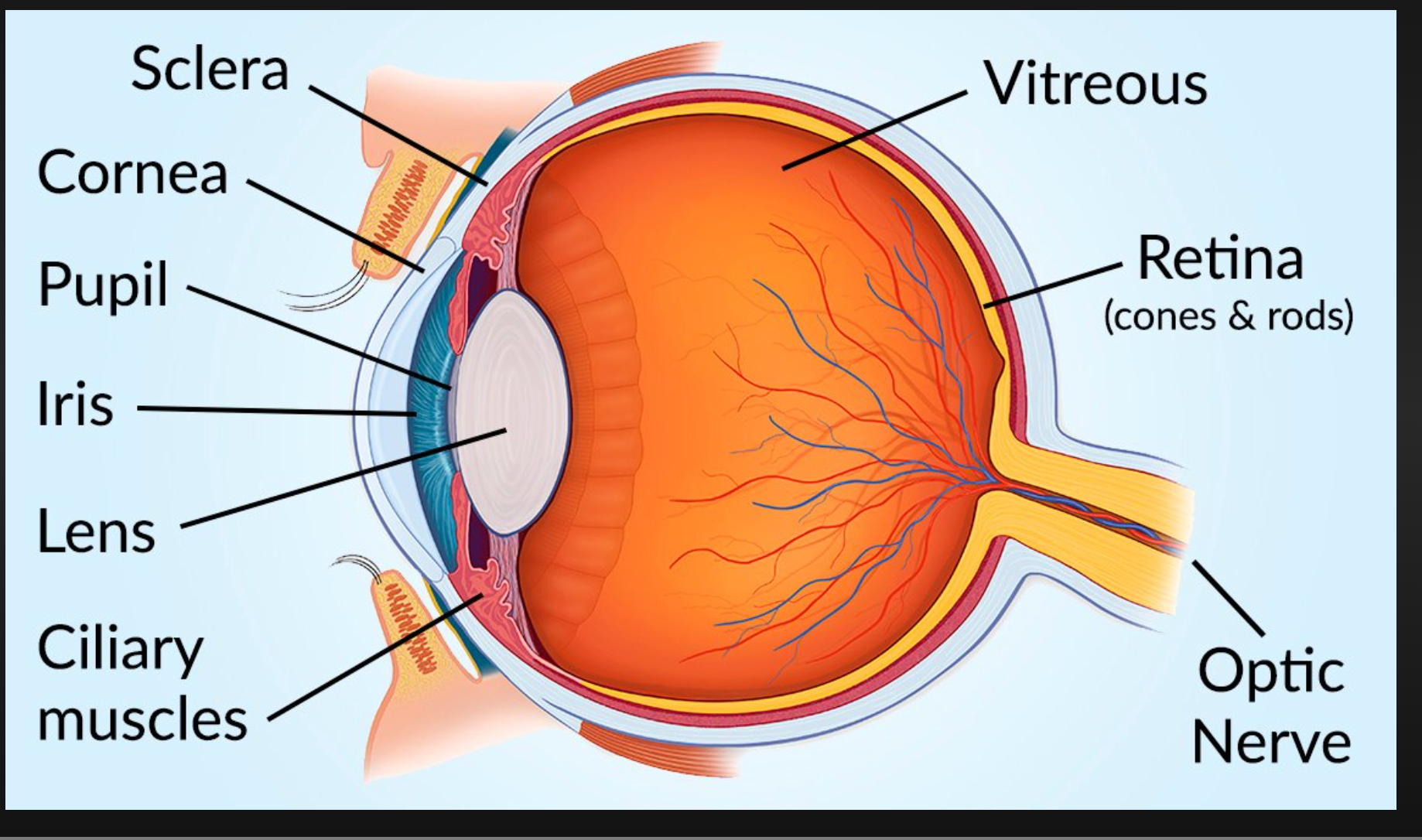
Your Eyes are Windows To Your Health Eyesight is one of the most important organs of our senses. Our eyes provide light, knowledge, beauty, and many other blessings. However, a time may come when an eye disease impacts your vision. One of the most common eye conditions that impacts millions of people is Cataracts. Cataracts are cloudy areas that form on the lens of your eye. As you get older, the proteins in your lens beak down, forming cloudy patches that affect your vision. You may experience symptoms such as double or blurry vision, eye strain to see clearly, a film over your sight (like looking through a dirty window), or total blindness in an eye. Cataracts can be easily corrected. There are various types of age-related Cataracts. Many people notice or are diagnosed with the condition in their 50s. Depending on a person’s eye health the condition can occur at any age. One of the leading causes of blindless in older adults is from Cataracts. The average Cataract surgery age is 65. The only way to treat Cataracts is to replace the optical lens. Now that you have some facts about Cataracts lets discuss why it’s important to care for your Cataracts. Cataracts are non-reversible and usually get worse with time. The worse the Cataracts becomes so does your quality of life. Your ability to see at a distance when walking, working, or performing the tasks of daily living will be impacted. For example, if you are walking and can’t identify an object or person clearly from a distance you may not be able to detect if danger is approaching. Seeing clearly gives you time to decide before encountering the situation, person, animal, or object. Let’s say you need to balance your budget but can’t see the numbers clearly. You may need to rely on someone else to manage your finances. Or you may write the wrong digit on a check, or miss important information that impacts what you pay. That's why it's important to be accountable for the health of your eyes. Having eye surgery can seem scary or bring on anxiety. Not knowing how your eyesight may be impacted after surgery can make you feel unsure about having the Cataracts removed. Or cause you to prolong getting the procedure. The question to ask yourself is if your health and quality of life is worth correcting your eyesight?
